We all at some point have had a wound, big or small, or even a surgery that after a few weeks started to look like normal skin and eventually barely noticeable. But that is not always the case. If you have a scar from a surgical procedure or other injuries it might interfere with how you move and even cause pain. A physical therapist might be able to help you manage those scars; but how? In order to answer that lets first go over a basic overview of the healing process.
After an injury, we go through four phases: hemostasis, inflammation, proliferation, remodeling. In the hemostasis phase, we get the blood coagulation that turns into a scab to stop bleeding; this happens within a minute. Right after that, during the inflammation phase, we see swelling, heat, pain, and redness. This phase also helps stop bleeding and creates an environment that prevents infection. Then comes the proliferative phase in which the body tries to rebuild the tissues. In this phase, the tissues contract trying to pull the wound edges together while new blood vessels are created to supply adequate nutrients. Also, collagen fibers are laid down during this phase. The collagen fibers laid down during the proliferative phase are disorganized but with the adequate stimulus, are reorganized turning the injured tissues into even stronger ones. This process is called the remodeling phase (also known as maturation phase), which takes place around three weeks after the initial injury lasting up to a year or more.
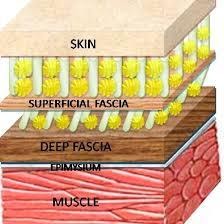
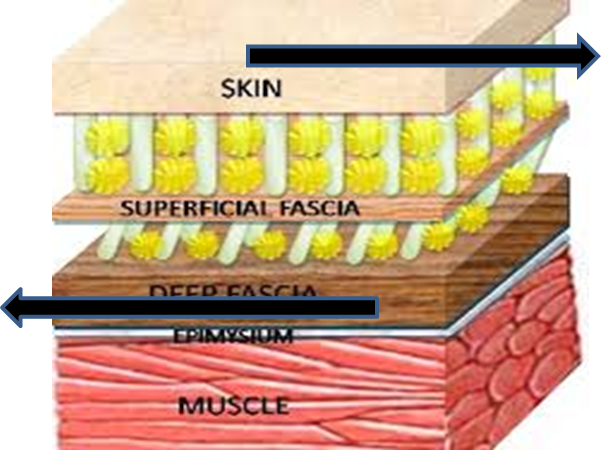
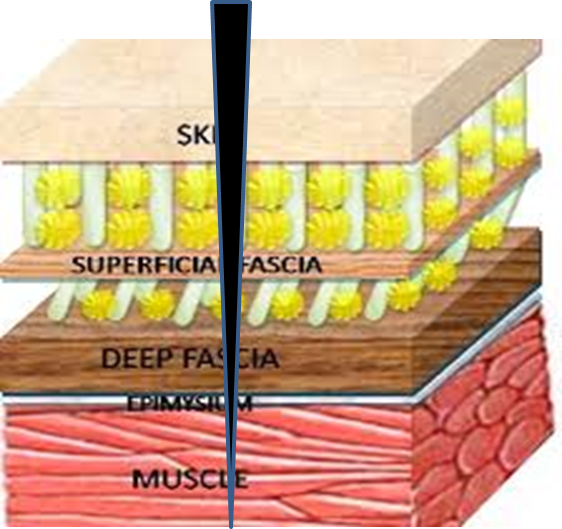
If everything goes smoothly, the wound area heals completely with life continuing as usual. But if at any of these phases, especially the proliferation or maturation phases, things do not go as expected, we might get scar formation that is less than optimal. The most common types of abnormal formations are atrophic, keloid, hypertrophic, and contracture. Any of these abnormal scar formations can cause problems with mobility, sensation, and even pain. When those collagen fibers are not properly laid down, they limit how much the tissues can move in a particular direction. It is like having a very very tight shirt and trying to raise the arm above the head, it pulls your arm down. This movement limitation is not only about a superficial restriction preventing general movement of the extremities, but also in between tissues. Under the skin we have different layers that glide against each other with every movement we make. When there is a surgical incision, all those layers are separated and are going to have to heal fusing together. But there are so many layers and fibers going in so many directions that they might develop adhesions or contractures thus limiting movement. Also, nerve endings might get entrapped, getting irritated, sensitized, and eventually causing pain.
The key here is to start moving those tissues early as soon as they are ready to be disturbed to promote a good realignment of the collagen fibers. If there is no movement stressing those tissues, there is no need for the body to change anything about them. That is when scar formation can deteriorate into less than optimal shapes causing mobility and pain problems. Massage is one treatment option to stimulate proper alignment and your therapist can teach you how to self-massage after discussing if the wound area is ready for it. Another option is the use of kinesiotaping to stretch the area in the direction your scar needs to have a sustained stimulus even when you are not in therapy. It basically consists of applying the taping pulling on the skin around the scar against the direction of most restriction. Dry needling with the use of specially designed needles can also help stretching and stimulating the realignment of collagen fibers. There are two different types of specially designed needles for this purpose. There are plenty of other things to take into consideration like diet, sleep, sun exposure, and more that should also be discussed with your therapist. The important thing to know is that if you have had a pain that can’t explain and have a scar or recent surgery, it might be a good idea to let your physical therapist know, it could be contributing to your problems and there are plenty of things we can do about it.